Can a diastasis recti be fixed without surgery?
Maybe. But you won’t know until you give it your best effort. I want you to keep in mind that there’s NO TIME LIMIT FOR HEALING!!! I’ve seen women who are 20 years postpartum and we’ve been able to fully close their diastasis. In reality, there isn’t an arbitrary time window. Once you give your body the right movement patterns that it needs and progressively challenge under load, it will start to respond. At any age and time postpartum!!
Diastasis recti can even be addressed to some extent during pregnancy. (Which is a bit off topic, but I’ve had clients who were concerned because their diastasis was rapidly opening up early in their pregnancy. Through the right corrective exercises, we were able to get their diastasis to actually decrease!)
Here’s an interview talking about why lateral breathing is so important for diastasis prevention during pregnancy.
That being said, it’s important to know that 100% of women have a diastasis recti at delivery. The goal is to help set you up for successful healing after childbirth without sacrificing other parts, like your pelvic floor.
Some individuals even have a diastasis recti without having any pregnancies. It still means looking at whether there are movement patterns or habits putting constant strain on their midline and affecting how their core functions.
How long will it take to heal a diastasis recti?
This can depend on your genetics and everything that is contributing to your diastasis. If the answer was just to “strengthen your abs,” everyone could be sent home with a simple handout. Unfortunately, it’s not that simple. Some people might have to address just one area, and others might need to work on various parts. It all depends on the individual.
It’s also important to assess how you determine it is healed. Technically, a diastasis that measures less than 2 fingers across with the ability to create tension is considered functionally healed.
Caveat: Not everyone can heal their diastasis. (But don’t automatically assume that’s you!!!) Sometimes the damage to the fascia is just too great. That being said, I’ve seen many, many, MANY women heal who were told by their doctor the only option they had was surgery. Even if you end up needing surgery, the work you do beforehand will help set you up for success afterward. Surgery doesn’t change patterns or strengthen muscles—it only tightens fascia. So even with surgery, you still need to work on pressure management strategies and learn how to load well through your core.
How to check a diastasis
Before we dive into all the anatomy and things to look at for helping improve your diastasis recti through exercise, let’s check your diastasis.
The width tells us how well your rectus (the “6-pack” up the front) is working. The depth tells us how well you can create tension across your linea alba and transfer load (looking at the function of your obliques and transverse abdominals). Decreasing the depth is more important than the width; but in the end, we want all of these muscles to work together!
How to check diastasis depth
To learn more, check out this article
https://www.coreexercisesolutions.com/how-to-check-for-diastasis-recti/
Studies show that back pain is not caused by or related to a diastasis (1). There is actually more correlation between pelvic floor issues and back pain (2). So if you’re thinking that getting your diastasis fixed will help your back, it might—but the research shows that it might not. Back pain often has more to do with how we move, breathe, and our muscle balance, which may be more affected by the strategies we use than the gap itself. That being said, you’re about to dive into some of those concepts, so keep reading!
Diastasis belts and braces
Some of you might be asking, “Why work this hard when you could simply throw on a brace and fix it, right?” Bracing can be useful when you’re very, very, very early postpartum, like the first few weeks, to give a bit of support. After those early days, it’s better to get the muscles involved to make a natural brace. Now, if someone’s symptoms are severe, I might want to use KT tape for diastasis recti to give their midline a little extra support. That’s more of a nudge in the right direction instead of a brace that could potentially put too much pressure down on their pelvic floor and cause issues. Plus, most of the people I see who use a brace go back to their starting point within a few days of removing it. So, let’s get your muscles stronger to work on dynamically supporting you!
For more on belly binding, check out this article
https://www.coreexercisesolutions.com/belly-binding/
5 posture improvements to help diastasis
Let’s talk through 5 postural concepts that can potentially be contributing factors to address for non-surgical diastasis treatment. Assessing these areas can help you determine specific exercises to correct your diastasis recti.
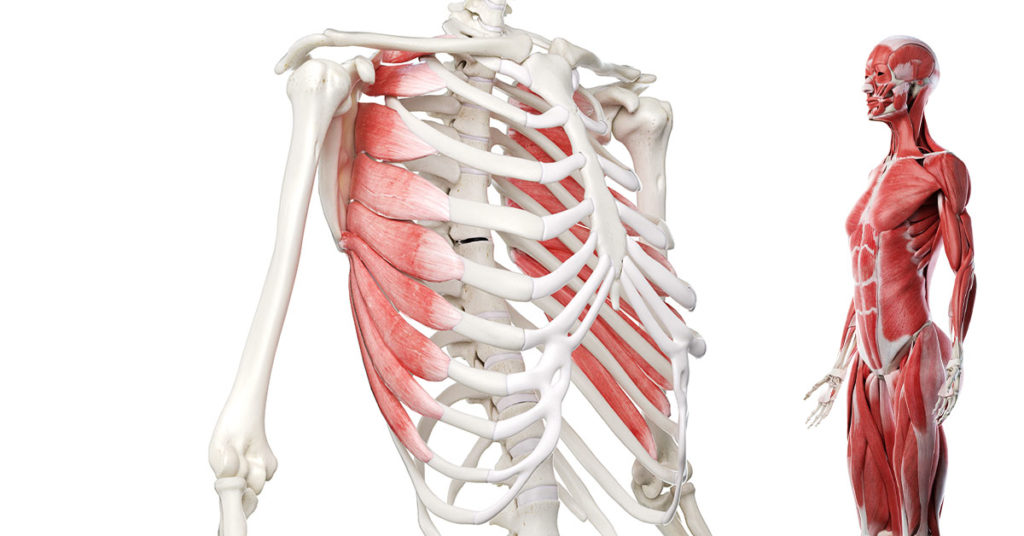
#1. Rib cage width for midline support
Being pregnant is tough, and as the baby grows and needs more room, our bodies accommodate by spreading the rib cage. All the changes that occur throughout pregnancy are actually pretty amazing! But without specific steps postpartum, some of those changes stick and can cause lingering issues like diastasis.
An easy way to know whether your rib cage has gone back to normal is your bra fit. Are you back into the same clasp setting as pre-pregnancy, or do your bras and sports bras all feel a bit snug? This means you might want to spend some time exploring your rib cage mobility and upper ab strength.
Tight bra problems
Rib cage width and obliques
Rib cage width can be fixed postpartum! It just depends on the muscles your body is using to move through life. Those who recruit more internal obliques tend to have a wider rib cage, and those who recruit more external obliques tend toward a narrower rib cage.
How your obliques affect rib cage angle
The cool thing about this observation is the issues I’ve seen linked to it. More internal oblique dominance is a finding I tend to see with diastasis. More external oblique dominance is a finding I tend to see with prolapse. In 2017, two studies (3) (4) came out that supported the things I was seeing. Love it when that happens! Women who tended to heal their diastasis faster had more risk of prolapse. The external obliques put pressure down on the pelvic floor, so having less dominant external obliques (and therefore the potential for more opening of the midline) could decrease prolapse risk postpartum. So, maybe a bit of a diastasis, especially early postpartum, has a protective effect for our pelvic floor. This also highlights how we don’t want to work on one area (like a diastasis) while sacrificing another (your pelvic floor).
Pelvic floor and diaphragm connection
What is pressure management?
Sometimes specific exercises can help increase external oblique strength, and other times a simple change of intention with an exercise can help work more external obliques.
Getting the external obliques to kick in to help heal a diastasis
Working on rib closure with a client
Half kneeling rotations with external obliques
Many of these exercises highlight working the concentric portion of the external obliques. However, strengthening through the full range can help with improved dynamic control, pressure management, and not gripping the upper abs.
It’s all how you unwind
Eccentric external obliques
Another consideration when working on increasing external oblique strength is that the person might need to improve their rib cage mobility. Those with a wide rib cage can have a lot of outward movement in their lower front ribs, but limited expansion elsewhere in the rib cage and limited movement coming back in. Doing some rib cage mobility work first can go a long way to help you avoid being in an internal tug of war with yourself.
Child’s pose breathing with overhead reach
Rib cage smash
Of course, we’re talking in generalizations here. For every 5 women who fit this pattern there will be 2 who don’t, but it’s good to keep in mind. In the end, it’s all about assessing and addressing the balance of your core engagement.
Correctly engage your abs
Bottom line to simplify: How does your bra strap fit? A little snug? That’s something I’d address with some rib cage mobility and increased concentric and eccentric external oblique strength (in both directions) before heading into surgery for your diastasis. Just make sure you’re creating a balance in your abs where you’re not closing a diastasis and sending the pressure down into your pelvic floor instead. This isn’t you? Then continue to look at other potential contributing factors.
#2. Diaphragm alignment and strength for diastasis healing
The diaphragm (breathing muscle) plays an incredibly important role in how our core looks and responds. Our rib cage helps to control how the diaphragm functions. If the diaphragm is in a more flattened position due to a wider rib cage, it can’t get a great contraction on an inhale. Without that great contraction, we’re much more likely to use a shallow breathing pattern with the inhale going up, which results in needing to over-recruit our abs to get a good exhale. This can send pressure down onto the pelvic floor, and it can also create a bit of a see-saw breathing pattern. This is where your back arches when you inhale and then you crunch on the exhale, resulting in an imbalance in what gets lengthened (and often putting too much stress out through a diastasis). It will reciprocally affect how we brace, creating more of a rectus-dominant bracing pattern.
Common breathing mistakes
Read more about why belly breathing is not optimal for healing
Instead, we want a nice, 360 degree breathing pattern for both the inhale and exhale so we don’t have to work so hard in either direction.
Hand feedback for breathing and bracing
You might be thinking, “Well, isn’t more work from our abs to breathe a good thing?”
Not at all! This overworking for breathing leaves the abdominals tight, and not tight in a good way! Tight in a way that creates excessive stress on your midline and perpetuates your diastasis.
Overworking our abs also means we’re often not getting good back-body expansion. Check out this video to learn how better lateral and back expansion can improve abdominal distension.
Rib cage mobility drills can be helpful here. Think of these as “knocking the rust off” the parts of the rib cage that are moving less on the inhale. When those parts move less, this can cause other parts (like your front lower ribs) to move more, putting constant strain on the diastasis. Mobility drills can also passively compress your rib cage and help the diaphragm lift up inside your thoracic cavity. This will give it a more optimal position to contract from and send pressure down with your inhale. Your abs will also not have to work so hard on the exhale to send the pressure back up.
The connection between diastasis and deep inner core muscles
Almost all the women I see with a diastasis either have a deep inner core that’s too tight, causing distention and that bread loaf appearance in the front, or they have a deep inner core that is kind of “offline” and doesn’t want to engage. The two can even go together.
Remember how I mentioned that the rectus controls the width, but not the depth? Sometimes you can be more rectus-dominant with your bracing due to tightness in the TAs and limited side expansion. This can lead to a decreased ability to maintain tension across your diastasis, which controls its depth.
When our deep inner core is responding with our system as a whole, you get a lot of give on your inhale into your sides and back. This is an eccentric lengthening of the muscle. This eccentric movement takes the stress off the midline and off the diastasis. It then creates a better position for your TAs to engage from for a more balanced brace, so you can see how creating a great 360-degree pattern can help set up better ab engagement.
What does it mean to be rectus dominant?
Dominant rectus and abs
To try and recruit more of your deep inner core, sometimes a simple change of intention can make a big difference. This includes making sure you’re not bracing out or scrunching down as you brace. This can not only put pressure out through your diastasis, but also down onto your pelvic floor. Instead, think of hollowing out or maintaining length in your spine while you brace. These tips will also help keep your pelvic floor safe while doing core work.
Lengthening abs to relieve pressure
Stop bracing out! Hollowing versus bracing
Being in more of a posterior pelvic tilt can help shorten your abs to make it easier to find them. That being said, you still want to make sure your abs are flattening with that engagement to make sure you’re bracing in a balanced way.
Flatten when you tuck
On the flip side, if you need help to avoid crunching and being rectus-dominant with your brace, a simple prop like a towel under your lumbar spine can help to keep length through your rectus and better find your TAs when you brace.
How to use a rolled towel
Bottom line to simplify: The abs should move out in all directions on your inhale as your diaphragm moves down. The women I see with a diastasis tend to either be in a shallow breathing pattern or a belly breathing pattern. Both can prevent healing. The good news is that it's something tangible to work on!! Improving the inhale will help set up a more balanced exhale and brace. With the brace, you want to make sure that it’s a balanced engagement. Sometimes we need different intentions or props to help balance out the system.
#3. Spinal alignment for diastasis healing
Without the expansion of the back part of the rib cage and diaphragm, a curve or high hinge point is often created in the spine just below the ribs at the segment where the diaphragm attaches.
If you’re unable to use your abs to stabilize your spine and pelvis, your diaphragm will become a primary stabilizing muscle which limits its ability to function well as a primary muscle of respiration. This brings us to another contributing factor to the high hinge point, which can be your psoas (hip flexors) and quadratus lumborum (back muscles) because they have similar insertion points as the back side of the diaphragm (5).
Now, before you go stretching your hip flexors, it’s important to understand if they are actually tight or if they’re just constantly hanging on, which makes them feel tight.
That being said, with either psoas or quadratus lumborum tightness, it’s important to look at what’s going on in your abs and hips. This way you’re addressing the actual problem to help get your hip flexors to let go.
Tight psoas
A high hinge point is often found in those with more of a swayback posture where they shift their rib cage back behind their pelvis (upper ab and chest gripping) or shove their hips forward below their rib cage (glute gripping and hanging on to hip flexors), often flattening out their lower lumbar curve. This can affect the constant tension out through our abs or create gripping in our abs or glutes, which can limit a diastasis from healing.
Plumb line assessment
Bottom line to simplify: Take a selfie in the bathroom mirror, and let’s analyze! Is your lumbar curve (curve toward your belly) down in your low back, or is the curve toward your belly higher, at your lower ribs? If it’s higher, this can be contributing to your diastasis. I almost always see this correlating with more of a gap or squishiness right above the belly button area.
Would your back hit a wall before your butt? Do your hips sit far forward? It’s time to investigate how your hips and lower abs are working.
#4. Lower abs and the pelvis for diastasis healing
When your lower abs are weak, your pelvis will either spill forward (an anterior pelvic tilt - APT) or you’ll grip in your glutes to provide stability, tucking your pelvis under (a posterior pelvic tilt - PPT). Being prone to living in either pelvic tilt can perpetuate a diastasis.
Being in an APT will position your abs in a more lengthened position from top to bottom, putting constant tension across a diastasis. Gripping glutes and going into a posterior pelvic tilt will shove the femurs forward in the socket, putting constant tension on the psoas and pressure forward out onto our abs. The tension at the psoas can contribute to a high hinge point and subsequent rib flare, further affecting core function.
Tight butt muscles and psoas
Along with lower abs, the glutes and hamstrings play a large role in positioning the pelvis, which can help with the resting position of the abs by allowing them to function in a more balanced way without having to overwork. (Laura mentioned this in her MomFit story as the final piece of the puzzle for her.)
The first step is being able to find the hamstrings in isolation. This can improve our resting pelvic position to help the attaching muscles function better and allow the glutes to be able to dynamically engage.
Unsticking the sacrum
Getting hamstrings without glutes to unstick the sacrum
How to recruit more glute med than piriformis
Then, rather than just working on each alone, you can do exercises that combine multiple concepts to get the most bang for your buck. Finding hamstrings while then working on a good 360-degree inhale can help reduce tension across the front of your abs and have a positive change on pelvis position, both of which will take stress off a diastasis (6).
Low back and belly reset
Using the hamstrings to address pelvic positioning first can help you better find your abs instead of your hip flexors
Following this path of exploring the pelvis, let’s take a further dive into what the glutes should be able to do. Having well-functioning glutes means we can eccentrically lengthen and contract our glutes in both directions, and we don’t compensate by moving into a different plane of motion than the one we’re trying to work in (such as moving into an APT or PPT while going into or coming out of a squat or deadlift). We need to have great balance in our glutes.
Why glutes need IR
Good versus bad IR
Being able to get the desired movements and relative motion at our hips in all planes will help maintain a good stack of our rib cage over our pelvis. This affects how our core, diaphragm, and pelvic floor function. Improving core strength also improves glute function, so once again, working on one area affects another (7).
Are your glutes initiating a squat, or is your back?
You can also assess how your glutes engage in a shortened position. Do you have (or get) a “butt dent” when you squeeze your glutes? Do you arch your back to squeeze, or do you have a flat bottom? These are all signs of untapped potential in your healing.
Glute activation test
Standing glute squeezes
Bottom line to simplify: Take a look at that bathroom selfie again. Without overarching your back to stick out your bottom (this is faking it, and creates back tightness in the process), take a look at your glutes.
Does your bottom look flat or have a butt dent? Or does it stick out with nice, round, full muscle without having to arch your back? Does one side look different than the other? We want a nice, round glute muscle on both sides, as best we can.
If you feel like you pass the eyeball test, try the tests above to see how your glutes actually function. Do you feel lengthening happening in your glutes as you squat or hinge? When you squeeze your glutes, do they stay full, or do you see a butt dent? How it looks is a starting point, but dynamic function gives you a better picture of what’s actually happening.
#5. Pelvic floor tightness for diastasis healing
A diastasis plays off the ability of the abs to fire as they should. The abs work in response to our habitual breathing pattern and our base of strength.
Pelvic floor tightness can decrease the ability of our diaphragm to go down. Remember how important diaphragm movement is for healing?
I also see pelvic floor tightness associated with hip imbalances, lack of glute strength, and lack of core stability. It’s the thing in the middle that acts to stabilize and support the spine and pelvis.
I’m not talking about crazy tightness, but just enough to decrease a good breathing pattern, affect how our glutes function, and decrease movement of the pelvic floor. The decreased movement of the pelvic floor can also affect its strength, and the deep abdominals work with the pelvic floor. Exploring and addressing pelvic floor tightness and how well you can engage the front of your pelvic floor can aid in your diastasis healing (8).
Release the pelvic floor
Front pelvic floor
Lower ab challenge
Think about how I mentioned the tight deep hip rotators and psoas connection, then the psoas connection to the diaphragm, and we’re back to the diaphragm and core connection. It’s all connected!
This can become a bit of a “chicken and the egg” situation with each of the areas feeding off of the other. Improving hip function and breathing can then affect how the pelvic floor functions, and vice versa.
Naturally lifting the pelvic floor
Bottom line to simplify: Take a big inhale down. Did you feel your pelvic floor give a little with your inhale? If not, you might have some pelvic floor tightness, and that might be part of the puzzle for improving your diastasis.
Breathe into your pelvic floor
Once you feel that your alignment is good and breathing is going well, it’s important to make sure you keep the right amount of intensity in your exercises and progressively overload them. Too much stress on your linea alba will delay healing and possibly make your diastasis worse. Too little stress, and the fascia won’t know that it needs to remodel. Why heal if the area never gets stressed?!
So, knowing when to modify is important. Here are a few videos looking at planks and when to increase the intensity to help your diastasis continue to improve.
Should you do planks with a diastasis?
3 common plank mistakes
In the end, some people still need surgery, which is fine! However, if you end up deciding to have surgery, the surgery itself won’t strengthen your abs or improve how they (or the rest of your body) functions. If you don’t address how you put stress out through your midline, then there’s a chance your body will create enough pressure to put extra stress through the next area of least resistance, potentially resulting in other pressure management issues such as prolapse, hernias, or a diastasis in another location. So, whether you have surgery or not, it’s important to look at correcting how we manage pressure, stop putting too much stress through the midline, and then progressively overload to help functionally heal a diastasis.
References:
- Sperstad JB, Tennfjord MK, Hilde G, Ellström-Engh M, Bø K. Diastasis recti abdominis during pregnancy and 12 months after childbirth: prevalence, risk factors and report of lumbopelvic pain. Br J Sports Med. 2016 Sep;50(17):1092-6. doi: 10.1136/bjsports-2016-096065. Epub 2016 Jun 20. PMID: 27324871; PMCID: PMC5013086.
- Dufour S, Vandyken B, Forget MJ, Vandyken C. Association between lumbopelvic pain and pelvic floor dysfunction in women: A cross sectional study. Musculoskelet Sci Pract. 2018 Apr;34:47-53. doi: 10.1016/j.msksp.2017.12.001. Epub 2017 Dec 9. PMID: 29268147.
- Smith MD, Coppieters MW, Hodges PW. Postural response of the pelvic floor and abdominal muscles in women with and without incontinence. Neurourol Urodyn. 2007;26(3):377-85. doi: 10.1002/nau.20336. PMID: 17279560.
- Bø K, Hilde G, Tennfjord MK, Sperstad JB, Engh ME. Pelvic floor muscle function, pelvic floor dysfunction and diastasis recti abdominis: Prospective cohort study. Neurourol Urodyn. 2017 Mar;36(3):716-721. doi: 10.1002/nau.23005. Epub 2016 Mar 31. PMID: 27037746.
- Penning L. Psoas muscle and lumbar spine stability: a concept uniting existing controversies. Critical review and hypothesis. Eur Spine J. 2000 Dec;9(6):577-85. doi: 10.1007/s005860000184. PMID: 11189930; PMCID: PMC3611424.
- Tenney HR, Boyle KL, Debord A. Influence of Hamstring and Abdominal Muscle Activation on a Positive Ober's Test in People with Lumbopelvic Pain. Physiother Can. 2013 Winter;65(1):4-11. doi: 10.3138/ptc.2011-33. PMID: 24381375; PMCID: PMC3563370.
- Chan MK, Chow KW, Lai AY, Mak NK, Sze JC, Tsang SM. The effects of therapeutic hip exercise with abdominal core activation on recruitment of the hip muscles. BMC Musculoskelet Disord. 2017 Jul 21;18(1):313. doi: 10.1186/s12891-017-1674-2. PMID: 28732494; PMCID: PMC5521096.
- Park H, Han D. The effect of the correlation between the contraction of the pelvic floor muscles and diaphragmatic motion during breathing. J Phys Ther Sci. 2015 Jul;27(7):2113-5. doi: 10.1589/jpts.27.2113. Epub 2015 Jul 22. PMID: 26311935; PMCID: PMC4540829.
Free Pelvic Floor and Diastasis Recti Course
What You Need to Know About Pressure Management
🎥 6 Video Lessons | 🕓 97 Min | 📑 PDF Downloads
Working with pregnant and postpartum clients/patients?
This 6-part course offers key takeaways on breathing, pelvic floor strengthening and diastasis recovery. Sign up and start learning today!