What is Diastasis Recti?
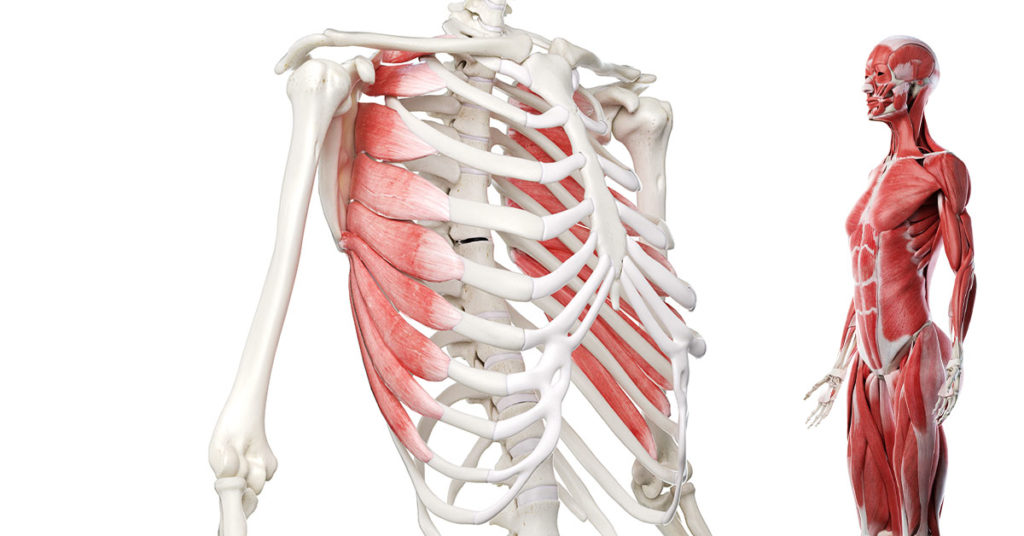
Diastasis recti is a thinning of the linea alba, which is the connective tissue where your rectus abdominis muscle (six pack ab muscles) meets in the middle from your pubic bone all the way up to your ribs. It is made up of the aponeurosis (think saran wrap) that is around the three lateral abdominal muscles -- transverse abdominals, external obliques, and internal obliques. These sheaths encase the rectus abdominis muscle and meet in the midline of the torso.
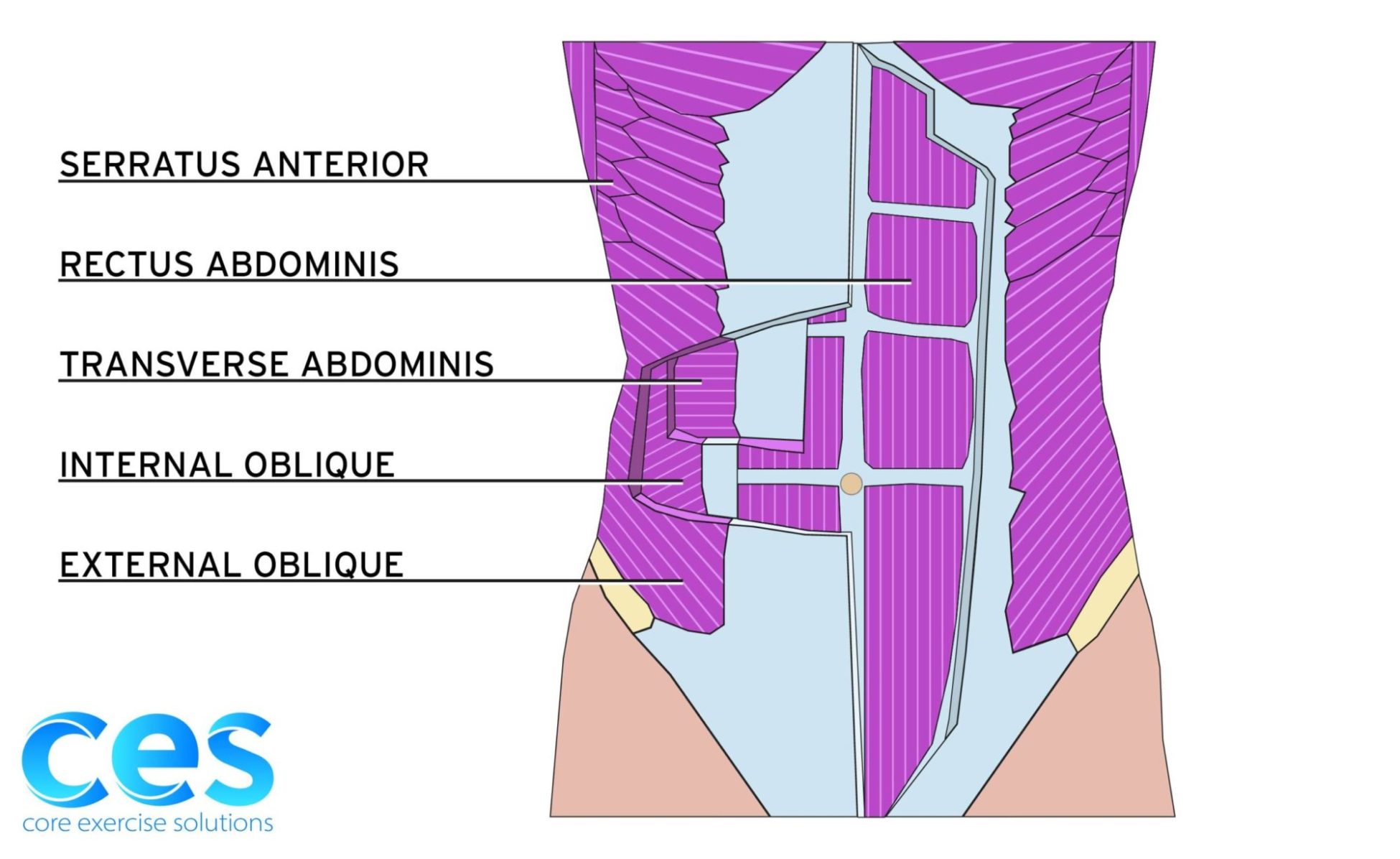
The fascia can be thinned above the navel, at the navel, below the navel, or along the entire length.
![Diastasis [Converted] Types of Diastasis Recti](https://www.coreexercisesolutions.com/wp-content/uploads/2021/03/Diastasis-Converted-scaled-e1615422125239.jpg)
Diastasis recti is most common in the postpartum population, but can also occur in other individuals (male or female) due to imbalances of abdominal muscle strength and engagement.

In pregnancy, there is a natural stretching and diastasis formation that is completely normal to accommodate a growing belly. In fact, according to Mota et al. (2015), 100% of women have a diastasis recti at their due date and 39% have it at 6 months postpartum. Sperstad et al. (2016) stated that 60% of women have diastasis at 6 weeks postpartum. Some women will heal their diastasis on their own while others will need specific exercises to help it heal, and sometimes surgery is needed if the fascia is compromised too much. Diastasis that seems really wide or deep at first still has the potential to heal, so don’t automatically assume you need surgery.
What Does Diastasis Recti Look Like?
Unless you have low body fat or an overly toned core, it is hard to see a diastasis without physically checking for it because your linea alba lies beneath any subcutaneous fat that is on your abdominal wall. Oftentimes people with a diastasis will complain of “looking pregnant” even if they’ve never been pregnant or it is months or years after having their child. This can vary based on the time of day (worse in the evening) or after eating big meals (abs aren’t strong enough to contain our insides) and with feelings of being bloated. You might also notice coning or doming along the midline of your abs when you go to sit up or perform other exercises or activities, or general weakness through your core. Some physicians check for a diastasis recti as part of a new mom’s 6 week postpartum check-up but other times they may not, and if you haven’t been pregnant, you might never have been checked for one. If you are having aches and pains elsewhere in your body, it can be helpful to assess for a diastasis to help determine if your pressure management and breathing and bracing strategy is an important component for your recovery. If a diastasis is more severe and there are concerns that a surgical intervention may be needed, ultrasound is used as the gold standard.
What Does Diastasis Recti Feel Like? How to Test for Diastasis Recti Postpartum?
A diastasis is assessed by looking at both depth and width as well as location, checking above and below the navel. Most often fingers will sink in along your linea alba (where not enough tension is created), but occasionally you can get a doming out or coning along your linea alba (where too much tension or pressure is created). Either version is still a positive finding of a diastasis. You can test yourself for a diastasis by following these simple steps:
- Start by rolling to your side and over to your back. Never sit straight up, always go from your side to put less pressure on your diastasis and PF (pelvic floor). We’re going to check in several places and make notes on this to compare later. The most important thing when measuring is how firm it is when you push down in the middle.
- Halfway between belly button and rib cage Find your belly button and your rib cage. Pick your head up. If you do feel a gap, how wide is this gap? Do your fingers squish in?
- Right above your belly button Pick up your head. Feel here, is there any gapping here? How far do your fingers go down? How many fingers wide is it?
- Below your belly button Pick up your head. Is it met with firmness, or is it soft and squishy?
- Adding in the breath What is your breathing system like? What is your PF is doing? This time I want you to think when you exhale, ribs in and down and PF comes up. What’s your gap like now? Does it get more squishy or more firm? We’re looking for the changes that happen here when you exhale and draw your PF up.
If you have a separation that is wider than 2 fingers and any softness in the linea alba, you will need specific exercises to help heal your diastasis. The depth or squishiness of diastasis is affected by your deep core (TAs and pelvic floor) and the width is affected by rectus strength. The location of a diastasis and the corresponding measurements can vary per individual, depending on how your breathing, bracing, and pressure management system works and also how areas above (shoulders) and below (hips) function. You want your bracing strategy to be a balance of both your superficial and deep core systems. If you have a diastasis that is initially more narrow but deeper, you’d rather have it be a little wider (still under 2 fingers) with no depth. A healed diastasis is firm or trampoline feeling for depth, and under 2 fingers in width.
Our pelvic floor can also play a huge role in the depth of your diastasis. It is important to make sure you aren’t putting too much pressure down when you’re trying to close your gap, while including breathing and bracing strategies to help bring firmness to your diastasis. It can initially be helpful to check the diastasis without any cuing, and then see how it might improve with the cuing of getting a great 360 degree inhale and then exhaling from the bottom up, feeling the lift of your pelvic floor and ribs and your abs coming down, in and together. If the diastasis improves with cuing, that tells you they already have the connections in place that just need to be reminded how to work together. This might be a faster process than if you have to build those connections to start.
If the cuing of bringing your ribs and abs down, in and together causes lower belly pooching, then you need to step back and work on your pressure management first, focusing more on creating a 360 degree inhale and balance in your abdominal engagement. This will make sure you aren’t putting too much pressure down onto your pelvic floor, making it vulnerable for injury, as you try to heal your diastasis.
How to Tell if you Have a Diastasis Recti?
Traditionally, this test is performed in a lying down position, but it is also important to test in other positions to help you determine if that position is hindering or helping your diastasis. Another reason a diastasis might not be improving is if you are either loading it too much or not loading it enough. If you end up having a wider or deeper gap while in a position such as a plank, then that exercise is putting strain on your diastasis and preventing it from improving. On the flip side, if while in this position your diastasis feels firm, then it is helping you heal your diastasis to get into the overloaded positions by helping your abs get stronger and more tolerant to higher loads and various conditions with improved resting tone.
How to Test Diastasis Recti While Pregnant?
Testing for a diastasis while pregnant depends on how far along you are in your pregnancy. Earlier on, or if you tend to create too little pressure, you will be more likely to have sinking in or a “ditch” along your linea alba.
As you get further along in pregnancy with a baby filling up the space, or if you tend to create too much pressure, you will have coning or doming where space between your linea alba pushes out.

How to Check for Diastasis Recti when Overweight?
You can assess a diastasis no matter your body size or type. If you have more abdominal tissue, you will still sink your fingers in at the midline and walk your fingers out to search for an edge or lip of your linea alba when relaxed, and then perform the test with your fingers at the edge to feel a change in that width and depth. If you are still unsure, feel free to reach out to a professional to help you with this assessment.
Diastasis Recti Prevention and Treatment
Diastasis recti is a diagnosis that can be treated, no matter how new or old the diastasis is. Sometimes it can be a matter of connecting and progressively overloading your breathing and bracing system, and other times you’ll need to rewire this system and work a bit more from the ground up. That might take a bit longer, but it is still doable. Either way, it’s about taking that good foundation and finding ways to continue strengthening its connections, making our abs stronger and giving the fascia an opportunity to heal.
Then sometimes we have to look at how the systems above and below our core are functioning. Most often, those with a higher diastasis need to address how their upper abs are working as well as their scapular and thoracic mobility and function, and those with a diastasis below the belly button will need to address lower abs as well as lower rib cage, hips, foot, and ankle function. Basically, be sure to check things out beyond how just your core is functioning, particularly if you have already worked on some foundations of breathing and bracing and still have a diastasis. If one area of the body isn’t moving well, it will make the movement happen from elsewhere, often creating more stress and strain across your diastasis
Finally, at times the fascia is just too thinned or stretched out, and in this case you will need surgery. However, learning proper strategies and working on imbalances leading into surgery will only set you up for more success post-surgery. Check out the following articles for more details about preventing and healing a diastasis:
- 3 Steps to Improve a Diastasis Recti
- Diastasis Recti Repair
- How to Heal Diastasis Recti Without Surgery
- Diastasis Recti During Pregnancy
This article was written by Anna Hammond, an amazing Physical Therapist that works at Core Exercise Solutions. You can find out more information about Anna here.
References:
- Mota, P., Pascoal, A.G., Carita, A.I., & Bø, K. (2015). Prevalence and risk factors of diastasis recti abdominis from late pregnancy to 6 months postpartum, and relationship with lumbo-pelvic pain. Manual Therapy, 20(1), 200-205, https://doi.org/10.1016/j.math.2014.09.002
- Sperstad, J. B., Tennfjord, M. K., Hilde, G., Ellström-Engh, M., & Bø, K. (2016). Diastasis recti abdominis during pregnancy and 12 months after childbirth: Prevalence, risk factors and report of lumbopelvic pain. British Journal of Sports Medicine, 50(17), 1092–1096. https://doi.org/10.1136/bjsports-2016-096065
Free Pelvic Floor and Diastasis Recti Course
What You Need to Know About Pressure Management
🎥 6 Video Lessons | 🕓 97 Min | 📑 PDF Downloads
Working with pregnant and postpartum clients/patients?
This 6-part course offers key takeaways on breathing, pelvic floor strengthening and diastasis recovery. Sign up and start learning today!